Because we’ve been able to prevent disease in the young animals and put off and/or manage some of the diseases that used to claim the lives of middle-age and older animals, we’re seeing more and more of our patients develop osteoarthritis as they age. This topic often comes up when we’re talking about how much exercise an elderly dog can handle, but osteoarthritis can also be an issue for middle-aged and even younger pets.
First, let’s talk about what osteoarthritis is. Osteoarthritis is inflammation in and around a joint that leads to changes of the bones and joint capsule. Osteoarthritis is a vicious circle involving multiple factors including cartilage damage, increased bone formation, thickening of the joint capsule, and a variety of hormonal and chemical changes. Some veterinarians and human physicians describe osteoarthritis as “organ failure,” and this really isn’t much of a stretch. When the cartilage and the joint capsule are no longer able to do the job of making mobility comfortable, pain is the result. The structures have failed to do their job.
“How would I know if my pet is developing osteoarthritis?”
Great question! Some signs you may see include: sluggishness, tiredness, decreased activity, reluctance to walk/run/climb stairs/play, lagging behind you on walks, reluctance to extend the hind legs, newly aggressive behavior, hiding/withdrawn behavior, or any behavior change. About 20% of all dogs in America deal with osteoarthritis in some form.
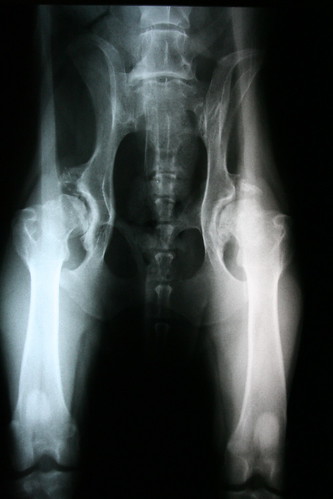 |
Sometimes osteoarthritis (also refered to as simply arthritis or degenerative joint disease) is a result of normal wear-and-tear associated with age. Sometimes it develops secondary to obesity. For other pets osteoarthritis is a result of an injury to a joint, such as a torn cruciate ligament in the stifle (knee) joint. And still for other pets, osteoarthritis forms as a result of joint abnormalities that are genetic in origin. An example of arthritis secondary to genetic changes is the pain that comes with hip dysplasia. In the radiograph shown here, the ball-and-socket joints of the hip ought to have nice, smooth surfaces but instead have very rough surfaces due to abnormal bone formation in and around the joint. This is the body’s inefficient way of dealing with the instability that comes with abnormal joint formation. These changes don’t make the joints more comfortable. In fact, they make the joint less comfortable.
All of these signs and symptoms are consistent with osteoarthritis. To be sure of the condition and to achieve a diagnosis, radiographs are necessary. X-rays give us a diagnosis, and they allow us to stage the condition and help us to set up appropriate expecations for an outcome and response.
So what can we do about osteoarthritis? The answer is actually… LOTS! In fact, the approach that we take with osteoarthritis is multi-modal therapy. This philosophy comes from the idea that no one treatment by itself is going to competely address the problem, because the underlying problem (osteoarthritis) often has a number of factors involved: instability of the joint, cartilage breakdown, inflammation of the joint capsule. Simply treating one of these factors will leave the other factor to worsen the arthritis, but by treating both factors, we can often deliver comfort and quality of life to our osteoarthritis patients.
 If joint instability is an issue, surgical stabilization is often required. For the purposes of our discussion today, we’ll just focus on medical therapy.
If joint instability is an issue, surgical stabilization is often required. For the purposes of our discussion today, we’ll just focus on medical therapy.
Using a variety of treatments often allows us to use less of each treatment compared to what we’d need to use if we selected just one form of treatment. This leads to another reason why multi-modal therapy is best. Because the treatments for osteoarthritis must be metabolized by some pathway in the body, giving treatments that pass through multiple parts of the body avoids taxing one specific pathway or organ.
Our top choices for the treatment of osteoarthritis are: Adequan, a non-steroidal anti-inflammatory drug (NSAID), nutritional support with Hill’s Prescription j/d, and supplementation with Dasuquin (glucosamine, chondroitin sulfate & avocado/soybean unsaponifiables [ASU]).
Adequan is an injectable treatment for osteoarthritis. It is the most forward-thinking of the treatments listed above because it prevents cartilage from breaking down and can actually help repair the joint, and is the only FDA-approved product with this claim. Adequan, in our experience, is best given early on in the arthritis process, before significant cartilage damage has taken place.
Rimadyl is our NSAID of choice. All NSAIDs impact the COX enzymes that contribute to joint inflammation. Of the treatments listed here, Rimadyl delivers the most noticable improvement the quickest. Non-steroidal anti-inflammatories should not be used in dogs with kidney disease or liver disease. We monitor all of our NSAID patients with routine bloodwork to be sure that they are metabolizing their treatment appropriately and to be sure that we are not causing a bigger problem than we are attempting to treat. For patients experiencing minor inflammation of the liver, there are good supplements that can be given with NSAIDs to promote liver health while allowing the patient to continue receiving the anti-inflammatory benefits of the NSAID. (Currently there are no NSAIDs with FDA approval for the treatment of feline arthritis.)
|
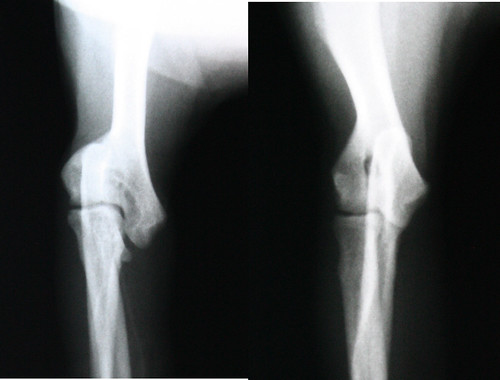
Dr. Ryan is a big fan of Royal Canin’s Mobility & Hill’s Prescription j/d. These therapeutic diets are saturated with omega-3 fatty acids which are vital to protecting cartilage, and they’re is both low-cal and high in L-carnitine, which helps dogs maintain a healthy weight. Dr. Ryan’s Pug, Betty, has a bone deformity of her upper forelimb that has resulted in significant joint pain. Betty is also the only patient at Cuyahoga Falls Veterinary Clinic that vomits on every NSAID (every one!). Her joint disease was discovered around 3 years of age, she was three-legged lame, and her prospects for comfort looked bleak because her body wouldn’t tolerate medical therapy. Therapeutic diets were relatively new when Betty’s problem was found, and Dr. Ryan (and his wife, Dr. Jenn) were open to trying it. They set very low expectations, though. “How was diet therapy going to make her want to use her lame leg?” they asked. Betty became a crazy, happy, four-legged Pug again in a short period of time! To test whether or not the diet was the definitive treatment, they took her off of it after several months, and she regressed to her three-legged status again. She’s been on Royal Canin’s Mobility years and is doing great!
Royal Canin’s Mobility is available in a feline formula! The treatment options for cats with osteoarthritis are very limited, so having this diet therapy is a very valuable tool.
Dasuquin for dogs and cats is a combination nutriceutical product that delivers the glucosamine and chondroitin sulfate that many of our pet-owners swear by in themselves. It also provides additional neutriceutical help that targets joint-inflammation from multiple angles. Nutrition is more important for joint disease than anyone used to recognize, and Dasuquin helps provide excellent nutrition-help in a chewable treat form.
And now we have a Therapeutic Laser for the treatment of arthritis, among other conditions. Therapeutic laser has demonstrated great success in relieving joint pain, and it is very easy to apply the treatment as both dogs and cats are very tolerant of the laser. We’re very excited about adding this in the coming months and we’ll have much to say about this when the time comes, so stay tuned!
Regular, controlled exercise cannot be ignored when discussion therapy for arthritis. If regular exercise is not part of the picture, joints will become stiff with time. Short leash-walks can do wonders to keep arthritic joints loose.
If you are interested in discussing how to help your cat or dog with arthritis, don’t hesitate to give us a call @ 330-929-3223. Our overall goal is to address your pet’s joint pain in a way that will provide comfort in a safe, effective way to maximize quality of life.
(Illustrations compliments of Pfizer Animal Health.)


The Cuyahoga Falls Veterinary Clinic | Animal Wellness | Medical Services | Pet Services
[…] to use stairs, she refused to play, and she was moving painfully. She was not responsive to non-steroidal anti-inflammatory therapy. And because she was a Boxer, I was thinking the worst: there must be an ugly cancer somewhere. […]
The Cuyahoga Falls Veterinary Clinic | Animal Wellness | Medical Services | Pet Services
[…] here and there over the course of Nanook’s life, and most recently, we’ve been managing arthritis. Nanook is a sore fellow when he’s not on his anti-inflammatories, but with them he’s a […]
The Cuyahoga Falls Veterinary Clinic | Animal Wellness | Medical Services | Pet Services
[…] the dog that was given twice the dose of cortisone for arthritis every day for over a year without any follow-up or monitoring (a violation of the VCPR) and […]
The Cuyahoga Falls Veterinary Clinic | Animal Wellness | Medical Services | Pet Services
[…] of dollars over the course of an animal’s life, particularly those battling heart disease or arthritis. At the Cuyahoga Falls Veterinary Clinic we use a variety of generic drugs in place of the name […]